Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
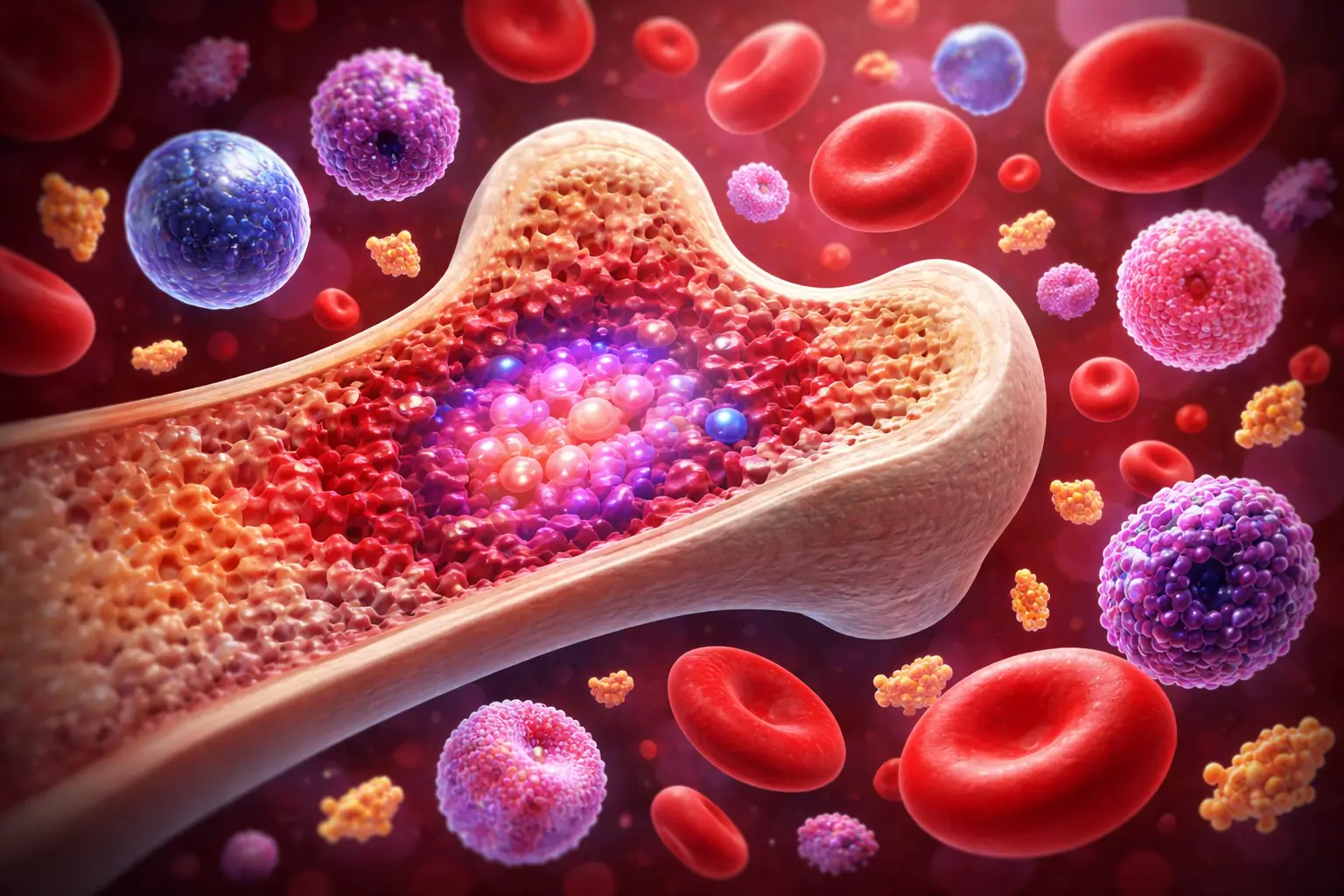
- Hematopoiesis = process of blood cell formation from stem cells in bone marrow
- Begins in yolk sac (embryo) → liver/spleen (fetus) → bone marrow (adult)
- All blood cells arise from one Hematopoietic Stem Cell (HSC)
- HSC → CMP (makes RBC, platelets, granulocytes) + CLP (makes lymphocytes)
- Regulated by EPO, TPO, G-CSF, IL-3 and other growth factors
- Defects → Anemia, Leukemia, Thrombocytopenia
Hematopoiesis is the continuous biological process by which all mature blood cells — red blood cells, white blood cells, and platelets — are produced from a single type of multipotent cell called the Hematopoietic Stem Cell (HSC). This process occurs primarily in the red bone marrow of adults and is essential for life.
/ hɪˌmætəʊpɔɪˈiːsɪs / | also spelled: Haematopoiesis / Hemopoiesis
Definition: Hematopoiesis is the process of formation, development, and differentiation of all cellular components of blood — including red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes) — from pluripotent hematopoietic stem cells.
🇮🇳 Hindi Meaning (हिंदी में): हेमेटोपोइसिस = रक्त कोशिका निर्माण की प्रक्रिया
(Rakt koshika nirmaan ki prakriya — blood cell formation process)
Hemopoiesis and hematopoiesis refer to the exact same biological process — blood cell formation. The difference is only in spelling. “Hematopoiesis” is used in American English, while “Haematopoiesis” is the British English spelling. “Hemopoiesis” is an older, simplified form. All three terms are used in textbooks.
| Term | Origin | Usage |
|---|---|---|
| Hematopoiesis | American English | Most common in modern textbooks |
| Haematopoiesis | British English | Used in UK/European journals |
| Hemopoiesis | Simplified form | Older texts, still acceptable |
All three mean the same thing. In your exam, either spelling is accepted. Use “Hematopoiesis” as standard.
Hematopoiesis is the broad umbrella process that produces ALL blood cells (RBC + WBC + platelets). Erythropoiesis is a sub-process within hematopoiesis that specifically produces only red blood cells. Simply put: Erythropoiesis is a part of Hematopoiesis.
| Feature | Hematopoiesis | Erythropoiesis |
|---|---|---|
| Scope | All blood cells | Only RBCs |
| Cells Produced | RBC, WBC, Platelets | Erythrocytes only |
| Stem Cell | HSC (pluripotent) | BFU-E → CFU-E |
| Hormone | Multiple (EPO, TPO, G-CSF) | Erythropoietin (EPO) |
| Organ | Bone marrow, liver (fetal) | Bone marrow (adult) |
| Relation | Broad process | Part of Hematopoiesis |
Hematopoiesis occurs in different organs at different stages of life. In the embryo, it starts in the yolk sac at 3 weeks. It shifts to the liver and spleen during fetal life (2nd–7th month). After birth, the red bone marrow becomes the primary and only site in healthy adults.
The earliest site of blood formation. Primitive erythroblasts are produced here. These are large, nucleated RBCs (unlike adult RBCs which have no nucleus).
Liver becomes dominant site by 3rd month. Spleen also participates. Definitive hematopoiesis begins here — both myeloid and lymphoid cells are produced. This is why liver is enlarged in fetal life.
Bone marrow takes over from the 5th month of fetal life and becomes the only site in adults. Red bone marrow is active; yellow marrow (fat) is inactive but can reactivate in emergencies.
In disease (e.g., severe anemia, myelofibrosis), liver and spleen can resume blood cell production in adults. This is abnormal and indicates bone marrow failure.
| Phase | Site | Age | Cells Produced |
|---|---|---|---|
| Mesoblastic | Yolk Sac | 3–8 weeks | Primitive RBCs (nucleated) |
| Hepatic | Liver, Spleen, Thymus | 2–7 months | RBCs, WBCs, Megakaryocytes |
| Myeloid | Bone Marrow | 5th month → Adult | All blood cells |
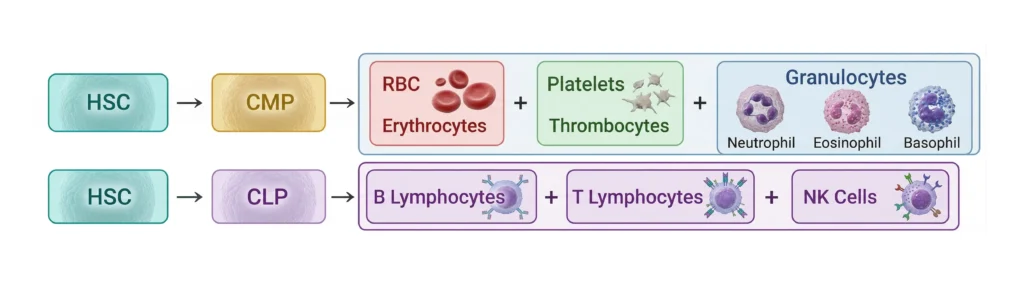
All blood cells come from one HSC (Hematopoietic Stem Cell). HSC divides into two main progenitor cells: CMP (Common Myeloid Progenitor) — which produces RBCs, platelets, and most WBCs — and CLP (Common Lymphoid Progenitor) — which produces lymphocytes (B cells and T cells).
ANALOGY
Think of the HSC as a master factory. The CMP wing makes goods for transport (RBCs), defense police (neutrophils, monocytes), and delivery trucks (platelets). The CLP wing trains security intelligence (lymphocytes). Both wings share the same factory building — the bone marrow.
| Progenitor | Produces | Hormone/Factor |
|---|---|---|
| HSC (Hematopoietic Stem Cell) | All blood cells — pluripotent | SCF, IL-3 |
| CMP (Common Myeloid Progenitor) | RBCs, Platelets, Neutrophils, Monocytes, Eosinophils, Basophils | EPO, TPO, G-CSF, M-CSF |
| CLP (Common Lymphoid Progenitor) | B cells, T cells, NK cells | IL-7, IL-2 |
Hematopoiesis follows a defined sequence: HSC self-renews and commits to a lineage, then progenitor cells proliferate and differentiate into precursor cells, which mature into functional blood cells. Each step is irreversible — once committed, a cell cannot return to an earlier stage.
| Stage | Term | Characteristics |
|---|---|---|
| 1 | Stem Cell (HSC) | Self-renewing, pluripotent, CD34+ marker |
| 2 | Progenitor Cell (CMP/CLP) | Limited self-renewal, lineage-committed |
| 3 | Precursor Cell | Morphologically identifiable, e.g. Myeloblast, Erythroblast |
| 4 | Mature Cell | Functional blood cell — RBC, WBC, Platelet |
Erythropoiesis is the production of red blood cells from stem cells in the bone marrow, stimulated by the hormone Erythropoietin (EPO) released by the kidneys in response to low oxygen (hypoxia). The full maturation cycle takes approximately 7 days.

Reticulocyte count is a direct measure of active erythropoiesis. Elevated reticulocytes = bone marrow responding to blood loss or hemolysis. Low reticulocytes in anemia = bone marrow not producing enough RBCs (aplastic anemia risk).
Leukopoiesis is the production of white blood cells. It includes granulopoiesis (for neutrophils, eosinophils, basophils from CMP) and lymphopoiesis (for B and T lymphocytes from CLP). G-CSF stimulates granulopoiesis and is used clinically in chemotherapy patients to boost WBC counts.
| WBC Type | Precursor | Growth Factor | Function |
|---|---|---|---|
| Neutrophil | Myeloblast → Myelocyte → Band → Neutrophil | G-CSF | Phagocytosis (bacterial) |
| Eosinophil | Eosinophil Myelocyte | IL-5 | Allergy, parasites |
| Basophil | Basophil Myelocyte | IL-3 | Histamine release |
| Monocyte | Monoblast → Promonocyte | M-CSF | Phagocytosis, becomes macrophage |
| B Lymphocyte | Lymphoid Stem Cell | IL-7 | Antibody production |
| T Lymphocyte | Thymus processed | IL-2, IL-7 | Cell-mediated immunity |
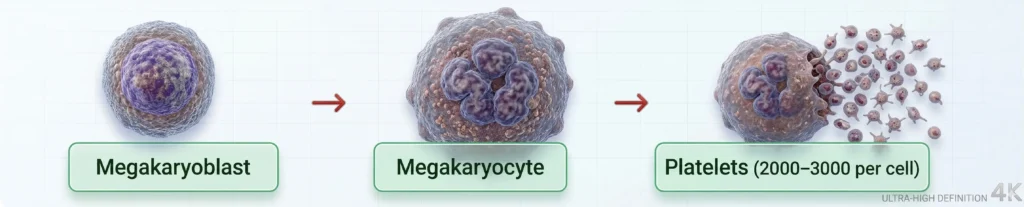
Thrombopoiesis is the production of platelets (thrombocytes) from large bone marrow cells called megakaryocytes. The hormone Thrombopoietin (TPO), produced by the liver and kidneys, stimulates megakaryocyte development. Each megakaryocyte produces 2,000–3,000 platelets.
Clinical Relevance
Low platelet count (Thrombocytopenia <150,000/µL) → bleeding risk. High count (Thrombocytosis >450,000/µL) → clotting risk. TPO is the target of drugs like eltrombopag used in ITP treatment.
Hematopoiesis is tightly regulated by cytokines and growth factors produced by stromal cells in the bone marrow. Key regulators include Erythropoietin (EPO) for RBCs, Thrombopoietin (TPO) for platelets, and G-CSF for granulocytes. Vitamins B12 and folic acid are also essential for proper cell maturation.
| Growth Factor / Hormone | Produced By | Stimulates |
|---|---|---|
| EPO — Erythropoietin | Kidneys (peritubular cells) | Erythropoiesis (RBC) |
| TPO — Thrombopoietin | Liver, Kidneys | Megakaryocyte / Platelet |
| G-CSF | Endothelium, Fibroblasts | Neutrophil production |
| M-CSF | Stromal cells | Monocyte production |
| IL-3 (Multi-CSF) | T cells | Multiple lineages |
| SCF (Stem Cell Factor) | Stromal cells | HSC proliferation |
| Vitamin B12 / Folic Acid | Diet | DNA synthesis for cell division |
| Iron | Diet / Absorption | Hemoglobin synthesis |
Normal blood cell counts vary by age and sex. The standard adult reference ranges are used in NABL-accredited laboratories and are aligned with WHO and CLSI guidelines. Any value outside these ranges triggers a critical value alert.
Complete Blood Count (CBC) — Normal Adult Reference Values
| Parameter | Male | Female | Unit |
|---|---|---|---|
| Hemoglobin (Hb) | 13.5–17.5 | 12.0–15.5 | g/dL |
| RBC Count | 4.5–5.9 | 3.8–5.2 | × 10⁶/µL |
| Hematocrit (PCV) | 41–53% | 36–46% | % |
| MCV | 80–100 | fL | |
| MCH | 27–33 | pg | |
| MCHC | 32–36 | g/dL | |
| WBC (TLC) | 4,000–11,000 | /µL | |
| Platelets | 150,000–450,000 | /µL | |
| Reticulocyte Count | 0.5–1.5% | % | |
Critical Values (NABL Alert Limits)
Hb <7 g/dL or >20 g/dL | WBC <2000 or >30,000/µL | Platelets <50,000 or >1,000,000/µL → Immediately inform the doctor.
Disorders of hematopoiesis can affect one or all blood cell lines. Decreased production causes cytopenias (anemia, leukopenia, thrombocytopenia), while uncontrolled proliferation causes leukemias. Understanding hematopoiesis helps MLT professionals identify abnormal cells on blood smears and interpret CBC results.
| Disorder | Lineage Affected | Lab Finding |
|---|---|---|
| Iron Deficiency Anemia | Erythroid | Low Hb, Low MCV, Low MCH, Microcytic hypochromic RBCs |
| Megaloblastic Anemia | Erythroid (B12/Folate) | High MCV, Macro-ovalocytes, Hypersegmented neutrophils |
| Aplastic Anemia | All lineages (HSC failure) | Pancytopenia, Hypocellular marrow |
| Acute Leukemia (AML/ALL) | Myeloid / Lymphoid | Blast cells >20%, High WBC, Low Hb, Low Platelets |
| Polycythemia Vera | Erythroid (excess) | High RBC, High Hb, JAK2 mutation |
| ITP | Platelet (immune destruction) | Low platelets, Normal marrow megakaryocytes |
| Myelofibrosis | All — fibrosis of marrow | Teardrop cells, Extramedullary hematopoiesis |
In the hematology lab, quality control (QC) ensures accuracy of CBC results. Internal QC (IQC) using commercially prepared controls must be run daily. Results are plotted on a Levey-Jennings chart. Westgard rules are used to identify random error (1:3s rule) and systematic error (2:2s, 4:1s rules).
| Error | Effect on Result | Prevention |
|---|---|---|
| EDTA clots in sample | Low platelet count | Proper mixing — 8 gentle inversions |
| Sample too old (>6h) | MCV increases, RBC decreases | Process within 2–4 hours |
| Wrong anticoagulant ratio | All indices affected | Fill tube to mark; 1:9 ratio (EDTA:blood) |
| Lipemic sample | False high Hb (spectrophotometric) | Saline replacement method |
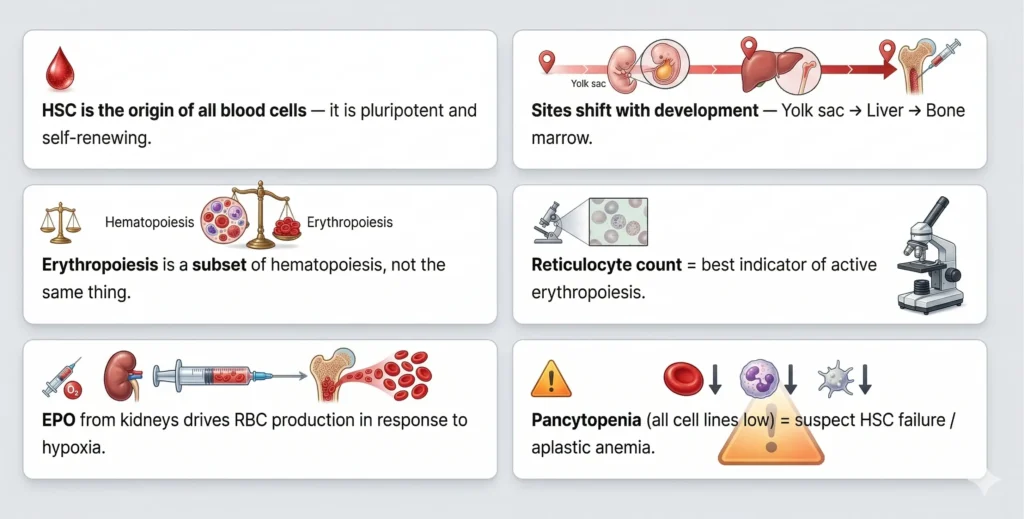
Hematopoiesis is the process of formation and development of all blood cells — red blood cells (RBCs), white blood cells (WBCs), and platelets — from hematopoietic stem cells (HSCs) located primarily in the red bone marrow of adults.
Hematopoiesis is the production of ALL blood cells. Erythropoiesis is specifically the production of RBCs only. Erythropoiesis is a sub-process within hematopoiesis. Think of it this way: Erythropoiesis ⊂ Hematopoiesis.
Three main stages by site: (1) Mesoblastic — Yolk sac (3–8 weeks); (2) Hepatic — Liver and Spleen (2nd–7th month fetal); (3) Myeloid — Bone marrow (from 5th fetal month through adult life). In adults, only red bone marrow is active.
हेमेटोपोइसिस का हिंदी अर्थ: रक्त कोशिका निर्माण की प्रक्रिया (Rakt koshika nirmaan ki prakriya). यह वह प्रक्रिया है जिसमें अस्थि मज्जा (bone marrow) में स्टेम सेल से सभी रक्त कोशिकाएं बनती हैं।
CMP (Common Myeloid Progenitor) gives rise to RBCs, platelets, neutrophils, eosinophils, basophils, and monocytes. CLP (Common Lymphoid Progenitor) gives rise to B lymphocytes, T lymphocytes, and NK cells. Both arise from the HSC.
Yolk sac (3–8 weeks), then Liver and Spleen (2nd–7th month), then Bone marrow (from 5th month onward).
HSC = Hematopoietic Stem Cell; CMP = Common Myeloid Progenitor; CLP = Common Lymphoid Progenitor.
Erythropoietin (EPO), produced by peritubular cells of the kidney in response to hypoxia.
Blood cell production occurring outside the bone marrow (in liver, spleen) in adults due to bone marrow failure. It is pathological in adults.
150,000–450,000/µL (1.5–4.5 × 10⁵/µL). (Source: WHO/CLSI)
One megakaryocyte produces approximately 2,000–3,000 platelets by shedding cytoplasmic fragments.
Pancytopenia (low RBC + WBC + platelets) indicates failure of the hematopoietic stem cell — suspect aplastic anemia, leukemia infiltration, or hypersplenism.
CD34+ (and Lin−, CD38−). CD34 is used in flow cytometry to identify and count HSCs, especially before bone marrow transplants.
Hematopoiesis is the foundation of all hematology. Understanding how blood cells form — from a single stem cell in the bone marrow, through the lineage of CMP and CLP, to mature RBCs, WBCs, and platelets — is essential for every DMLT/BMLT student. It helps you interpret CBCs, identify disorders, and perform quality lab work. Master this topic and you master hematology.